Normally, 7-8% of human body weight
is from blood. In adults, this amounts to 4.5-6 quarts of blood.
This essential fluid carries out the critical functions of transporting
oxygen and nutrients to our cells and getting rid of carbon dioxide,
ammonia, and other waste products. In addition, it plays a vital role
in our immune system and in maintaining a relatively constant body
temperature. Blood is a highly specialized tissue composed of more
than 4,000 different
kinds of components. Four of the most important ones are red cells,
white cells, platelets,
and plasma. All humans produce these blood
components--there are no populational or regional differences.
Red
Cells
 |
|
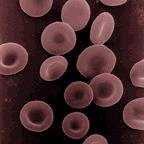
| Human
erythrocytes or "red cells" (cell diameter about .0003 inches) |
Red cells, or erythrocytes
![]() , are
relatively large microscopic cells without nuclei. In this latter trait,
they are similar to the primitive
prokaryotic cells of bacteria. Red cells normally
make up 40-50% of the total blood volume. They transport oxygen from the
lungs to all of the living tissues of the body and carry away carbon dioxide.
The red cells are produced continuously in our bone marrow from
stem cells at a rate of about 2-3
million cells per second.
Hemoglobin
, are
relatively large microscopic cells without nuclei. In this latter trait,
they are similar to the primitive
prokaryotic cells of bacteria. Red cells normally
make up 40-50% of the total blood volume. They transport oxygen from the
lungs to all of the living tissues of the body and carry away carbon dioxide.
The red cells are produced continuously in our bone marrow from
stem cells at a rate of about 2-3
million cells per second.
Hemoglobin
![]() is the gas transporting protein molecule that makes up 95% of a
red cell. Each red cell has about 270,000,000 iron-rich hemoglobin molecules. People who
are anemic generally have a deficiency in red cells, and subsequently feel
fatigued due to a shortage of oxygen. The red color of blood
is primarily due to oxygenated red cells. Human fetal hemoglobin
molecules differ from those produced by adults in the number of amino acid
chains. Fetal hemoglobin has three chains, while adults produce only
two. As a consequence, fetal hemoglobin molecules attract and
transport relatively more oxygen to the cells of the body.
is the gas transporting protein molecule that makes up 95% of a
red cell. Each red cell has about 270,000,000 iron-rich hemoglobin molecules. People who
are anemic generally have a deficiency in red cells, and subsequently feel
fatigued due to a shortage of oxygen. The red color of blood
is primarily due to oxygenated red cells. Human fetal hemoglobin
molecules differ from those produced by adults in the number of amino acid
chains. Fetal hemoglobin has three chains, while adults produce only
two. As a consequence, fetal hemoglobin molecules attract and
transport relatively more oxygen to the cells of the body.
White
Cells
White cells, or leukocytes
![]() , exist in
variable numbers and types but make up a very small part of blood's volume--normally
only about 1% in healthy people. Leukocytes are not limited to blood. They occur
elsewhere in the body as well, most notably in the spleen, liver, and lymph
glands. Most are produced in our bone marrow from the same kind
of stem cells that produce red blood cells. Others are produced in the
thymus gland, which is at the base of the neck. Some white
cells (called lymphocytes
, exist in
variable numbers and types but make up a very small part of blood's volume--normally
only about 1% in healthy people. Leukocytes are not limited to blood. They occur
elsewhere in the body as well, most notably in the spleen, liver, and lymph
glands. Most are produced in our bone marrow from the same kind
of stem cells that produce red blood cells. Others are produced in the
thymus gland, which is at the base of the neck. Some white
cells (called lymphocytes
![]() )
are the first responders for our immune system. They seek out, identify,
and bind to alien protein on bacteria,
viruses, and fungi
so that they can be removed.
Other white cells (called granulocytes
)
are the first responders for our immune system. They seek out, identify,
and bind to alien protein on bacteria,
viruses, and fungi
so that they can be removed.
Other white cells (called granulocytes
![]() and macrophages
and macrophages
![]() )
then arrive to surround and destroy the alien cells. They also
have the function of getting rid of dead or dying blood cells
as well as foreign matter such as dust and asbestos. Red
cells remain viable for only about 4 months before they are removed from the
blood and their components recycled in the spleen. Individual white
cells usually only last 18-36 hours before they also are removed, though some
types live as much as a year. The description of white cells presented
here is a simplification. There are actually many specialized
sub-types of them that participate in different ways in our immune
responses.
)
then arrive to surround and destroy the alien cells. They also
have the function of getting rid of dead or dying blood cells
as well as foreign matter such as dust and asbestos. Red
cells remain viable for only about 4 months before they are removed from the
blood and their components recycled in the spleen. Individual white
cells usually only last 18-36 hours before they also are removed, though some
types live as much as a year. The description of white cells presented
here is a simplification. There are actually many specialized
sub-types of them that participate in different ways in our immune
responses.
Platelets
 |
|
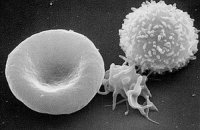
| erythrocyte (left),
thrombocyte (center), and leukocyte (right) |
Platelets
![]() , or
thrombocytes
, or
thrombocytes
![]() , are cell
fragments without nuclei that work with blood clotting chemicals at the site of wounds.
They do this by adhering to the walls of blood vessels, thereby plugging the rupture in
the vascular wall. They also can
release coagulating chemicals which cause clots to form in the blood that
can plug up narrowed blood vessels. Thirteen different blood clotting
factors, in addition to platelets, need to interact for clotting to occur.
They do so in a cascading manner, one factor triggering another.
Hemophiliacs lack the ability to produce either blood factor 8 or 9.
, are cell
fragments without nuclei that work with blood clotting chemicals at the site of wounds.
They do this by adhering to the walls of blood vessels, thereby plugging the rupture in
the vascular wall. They also can
release coagulating chemicals which cause clots to form in the blood that
can plug up narrowed blood vessels. Thirteen different blood clotting
factors, in addition to platelets, need to interact for clotting to occur.
They do so in a cascading manner, one factor triggering another.
Hemophiliacs lack the ability to produce either blood factor 8 or 9.
Platelets are not equally effective in clotting blood throughout the entire day. The body's circadian rhythm system (its internal biological clock) causes the peak of platelet activation in the morning. This is one of the main reasons that strokes and heart attacks are more common in the morning.
Recent research has shown that platelets also help fight infections by releasing proteins that kill invading bacteria and some other microorganisms. In addition, platelets stimulate the immune system. Individual platelets are about 1/3 the size of red cells. They have a lifespan of 9-10 days. Like the red and white blood cells, platelets are produced in bone marrow from stem cells.
Plasma
Plasma
![]() is the relatively clear,
yellow tinted water (92+%), sugar, fat, protein and salt
solution which carries the red
cells, white cells, and platelets. Normally, 55% of our blood's volume is made up of
plasma. As the heart pumps blood to cells throughout the body, plasma brings nourishment
to them and removes the waste products of metabolism. Plasma also contains blood clotting factors, sugars, lipids,
vitamins, minerals, hormones, enzymes,
antibodies, and other
proteins. It is likely that plasma
contains some of every protein produced by the body--approximately 500 have been identified in
human plasma so far.
is the relatively clear,
yellow tinted water (92+%), sugar, fat, protein and salt
solution which carries the red
cells, white cells, and platelets. Normally, 55% of our blood's volume is made up of
plasma. As the heart pumps blood to cells throughout the body, plasma brings nourishment
to them and removes the waste products of metabolism. Plasma also contains blood clotting factors, sugars, lipids,
vitamins, minerals, hormones, enzymes,
antibodies, and other
proteins. It is likely that plasma
contains some of every protein produced by the body--approximately 500 have been identified in
human plasma so far.
|
This link takes you to an external website. To return here, you must click the "back" button on your browser program. (length = 53 secs) |
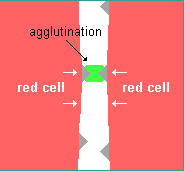
Agglutination
Sometimes when the blood of two people is mixed
together, it
clumps or forms visible islands in the liquid plasma--the red cells become attached to one
another. This is agglutination
![]() .
.
 |
 |
|
|---|---|---|
Unagglutinated blood smear |
Agglutinated blood |
When different types of blood are mixed within the body, the reaction can be a bursting of the red cells as well as agglutination. Different types of blood are recognized on the molecular level and sometimes rejected by being destroyed and ultimately filtered out by the kidneys in order to expel them from the body along with urine. In the case of a transfusion mistake, there can be so much of the wrong type of blood in the system that it can result in kidney failure and death. This is due to the fact that when the kidneys try to filter the blood, they essentially become clogged as they are overwhelmed and cease being effective filters. Additionally, there is a rapid depletion of blood clotting factors which causes bleeding from every body orifice. In the United States, about 1 in 12,000 units of whole blood transfused is given to the wrong person. Depending on the blood types of the donor and the recipient, this can result in death or no problems at all.
The
compositional difference between blood types is in the specific kinds of
antigens
![]() found on the surface
of the red cells. Antigens are relatively large protein molecules that provide the biological signature
of an individual's blood type.
found on the surface
of the red cells. Antigens are relatively large protein molecules that provide the biological signature
of an individual's blood type.
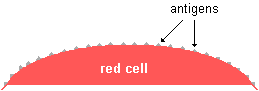 |
(not actual shape or size of antigens) |
Within
blood, there are substances called antibodies
![]() which
distinguish particular antigens from others, causing bursting or agglutination
of the red cells when
alien antigens are found. The antibodies bind to the antigens. In
the case of agglutination, the antibodies "glue" together the antigens from different
red cells thereby sticking the red cells together (as shown below on the right).
which
distinguish particular antigens from others, causing bursting or agglutination
of the red cells when
alien antigens are found. The antibodies bind to the antigens. In
the case of agglutination, the antibodies "glue" together the antigens from different
red cells thereby sticking the red cells together (as shown below on the right).
| Antibodies seeking specific antigens | Antibodies agglutinating red cells | |
|
|
 |
|
(not actual shape or size of antigens and antibodies) |
||